How excess fuel, insulin resistance, and poor metabolic flow lead to Non-Alcoholic Fatty Liver Disease
Most people hear the term fatty liver and assume the problem is simple.
There’s fat in the liver.
But the real story is more interesting—and more hopeful.
Non-Alcoholic Fatty Liver Disease (NAFLD) is not just fat accumulation. It’s a metabolic traffic jam.
The liver becomes overwhelmed with energy it cannot properly process.
When fuel arrives faster than the liver can burn it, store it, or export it, the excess begins accumulating inside liver cells as fat.
Over time this can lead to:
• liver inflammation
• insulin resistance
• metabolic syndrome
• eventually type 2 diabetes
But to understand why this happens, we need to understand the role the liver plays in metabolism.
The Liver: The Body’s Metabolic Control Center
The liver is one of the most active metabolic organs in the body.
It helps regulate:
• blood sugar
• fat metabolism
• cholesterol production
• glycogen storage
• detoxification
• hormone signaling
Nearly everything you eat passes through the liver first.
Under normal conditions the liver handles this workload easily.
It can:
• store glucose as glycogen
• burn fatty acids for energy
• export fats into circulation
• convert nutrients into usable fuel
Problems begin when energy arrives faster than the system can process it.
When that happens, the liver starts storing the excess.
The Three Main Pathways That Fill the Liver With Fat
Fatty liver usually develops through three overlapping metabolic pathways.
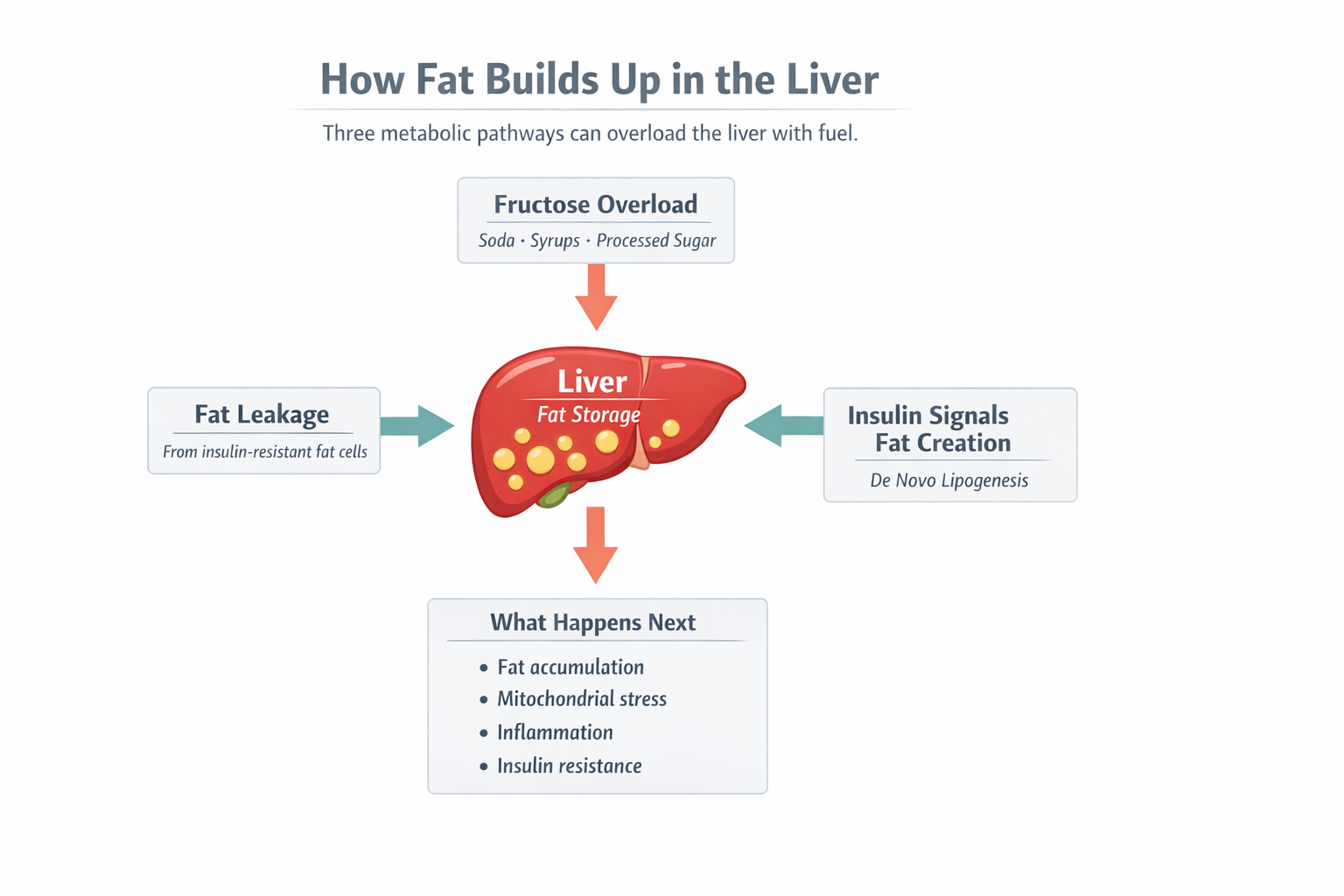
1. Chronic Insulin Signals the Liver to Make Fat
When insulin remains elevated for long periods, the liver activates a process called:
De novo lipogenesis
This literally means “new fat creation.”
In this pathway, excess carbohydrates are converted into fatty acids inside the liver.
Normally these fats are packaged into particles called VLDL and exported into circulation.
But when fat production exceeds the liver’s ability to export it, the fat begins accumulating inside liver cells.
This is one reason insulin resistance and fatty liver often appear together.
2. Fat Overflow From Insulin-Resistant Fat Cells
Fat tissue normally stores energy safely.
But when fat cells become insulin resistant, they begin releasing fatty acids into the bloodstream.
Those fatty acids travel directly to the liver.
Now the liver must deal with energy coming from multiple directions:
• fat from food
• fat created inside the liver
• fatty acids released from body fat stores
Eventually the system becomes overloaded.
3. Fructose Overload
Fructose is processed differently than most nutrients.
Unlike glucose, which can be used throughout the body, fructose is metabolized primarily by the liver.
When fructose intake becomes excessive—especially from sweetened beverages and processed foods—the liver converts much of it into fat.
This pathway can move quickly because fructose bypasses several metabolic checkpoints.
But an important distinction must be made here.
Whole fruit rarely causes this problem.
Fruit arrives packaged with:
• fiber
• water
• micronutrients
• slower absorption
These factors slow how quickly fructose reaches the liver.
Liquid sugars—sodas, syrups, and ultra-processed foods—deliver fructose in a way the body was never designed to handle.
They hit the liver all at once.
What Happens Once Fat Builds Up
When fat accumulates inside liver cells, several downstream problems begin to develop.
Mitochondrial Stress
The liver attempts to burn the excess fat through mitochondrial oxidation.
But fat metabolism requires large amounts of oxygen and healthy, efficient mitochondria.
When fatty acids arrive faster than mitochondria can process them—or when oxygen delivery is poor—the system begins to struggle.
Electrons start leaking from the metabolic pathways that generate energy.
Those leaks form reactive oxygen species, which create oxidative stress inside liver cells.
Over time this oxidative stress damages mitochondria and further weakens the liver’s ability to process incoming fuel.
The result is a vicious cycle:
Less efficient mitochondria → less fat processing → more fat accumulation.
Inflammation
Fat accumulation activates inflammatory signaling within the liver.
These signals spread throughout the body and worsen insulin resistance.
This is why NAFLD is strongly linked to:
• obesity
• insulin resistance
• type 2 diabetes
• cardiovascular disease
Rising Blood Sugar
Normally insulin signals the liver to stop producing glucose.
But when the liver becomes insulin resistant, it continues releasing sugar into the bloodstream even when blood sugar is already elevated.
This contributes to chronically high glucose levels.
The Cardiovascular Connection
Fat metabolism is highly dependent on oxygen.
And oxygen delivery depends on circulation and cardiovascular fitness.
If circulation is poor, tissues receive less oxygen. When oxygen is limited, the body cannot efficiently burn fat.
This means fatty acids remain in circulation longer and are more likely to accumulate in organs like the liver.
This is one reason fatty liver is strongly associated with low aerobic fitness and poor metabolic health.
Improving cardiovascular capacity improves oxygen delivery throughout the body.
Better oxygen delivery allows mitochondria to burn fuel more efficiently.
And when the body becomes better at burning fuel, less of that fuel ends up stored in the liver.
This is why improving cardiovascular health is one of the most powerful interventions for fatty liver.
Why Movement Helps So Much
Movement helps relieve the metabolic traffic jam.
Exercise:
• increases mitochondrial density
• improves oxygen utilization
• increases fatty acid oxidation
• improves insulin sensitivity
• lowers circulating triglycerides
• increases glucose uptake by muscle
Muscle becomes a fuel sink.
Instead of excess energy accumulating in the liver, it gets burned by working muscle.
The Exercise Bodyweight Daily (EBD) system fits perfectly here.
Frequent movement continually clears fuel from circulation.
When fuel has somewhere to go, the liver is no longer forced to store it.
Why Nutrition Structure Matters
Dietary structure also plays a major role in preventing fatty liver.
The nutritional principles used in AW Fitness Club naturally reduce metabolic overload.
For example:
Whole foods slow digestion and regulate blood sugar.
Fruit provides natural sugars buffered by fiber and water.
Hydration supports metabolic processes and detox pathways.
Intermittent fasting windows reduce chronic insulin exposure.
Structured meals prevent constant grazing.
Together these habits reduce the steady flood of energy hitting the liver throughout the day.
The Deeper Truth
Fatty liver is often described as a liver disease.
But in many cases, the liver is simply the organ forced to handle metabolic overflow.
The real issue is systemic:
• excess fuel
• insulin resistance
• poor metabolic flexibility
• low movement
• reduced mitochondrial capacity
When the metabolic environment improves, the liver often improves with it.
The liver is remarkably resilient.
Once the traffic clears, it can recover.
The Fitness Index Perspective
From the Fitness Index lens, fatty liver is not about avoiding one nutrient or blaming a single food.
It’s about restoring metabolic flow.
Movement creates energy demand.
Muscle burns fuel.
Structure regulates insulin.
And when metabolism begins moving again, the liver no longer has to store the excess.
Fatty liver is not caused by eating fruit.
It’s caused by a metabolism that has nowhere to put the energy it receives.
Restore movement.
Restore structure.
Restore metabolic flow.
And the liver often begins to heal.


